[Note: this post was originally published at the lovely Julie Hecht's Dog Spies blog at Scientific American.]
Where
I live, in America, it’s taken for granted that responsible owners spay
or neuter their dogs. The population of homeless animals is still large
enough that risking an unwanted litter is, to many owners, unthinkable.
And spay/neuter is just what people do. But two papers were
published, in 2013 and 2014, suggesting that these widely accepted
surgical procedures may lead to increased long-term risk of certain
kinds of cancers. These studies ignited a debate which had been
smouldering for years: are there unwanted health consequences associated
with altering a dog’s levels of estrogen or testosterone?
The 2013 paper
looked at Golden Retrievers. The authors reviewed data from veterinary
hospitals, comparing Goldens who were diagnosed with various diseases,
those who were not, and the spay/neuter status of each group; they found
a correlation between spaying or neutering and cancers such as
osteosarcoma, hemangiosarcoma, and mast cell cancer. The 2014 paper
used a voluntary Internet-based survey to perform a similar
investigation in the Vizsla breed. They also found correlations between
spay/neuter status and mast cell cancer, hemangiosarcoma, and lymphoma.
These are scary results, but I caution that studying the causes of
multi-factorial diseases like cancer is incredibly challenging. Take the
Golden Retriever study, a retrospective study using data from a
veterinary referral hospital. This study was limited to dogs whose
owners chose to bring them to a relatively expensive referral hospital.
This is the kind of place where you take your pet when he has cancer and
you are willing to spend a fair amount of money to help him. As a
result, this hospital’s records probably provide a great source of data
on companion animals living with concerned owners, particularly owners
who have provided excellent medical care for much or all of the animal’s
life. However, this hospital’s records are less likely to provide data
on animals whose owners have provided sub-optimal care. This kind of
bias in sample selection can have a significant effect on the findings
drawn from the data.
The Vizsla study used an Internet-based survey instead of hospital
records. Like the Golden Retriever study, this study could have found
itself with a biased sample of very committed dog owners, in this case
owners who engaged in dog-focused communities online and who had enough
concern about the health of the breed to fill out a survey. This study
additionally suffered from a lack of verified data; owners were asked to
give medical details about their dogs and may have misremembered or
misinterpreted a past diagnosis.
Don’t get me wrong – these were both important studies, and they did
their best with the available resources. I applaud both sets of authors
for putting this information out there. But the studies both have their
limitations, which makes their findings difficult to trust or generalize
to other populations of dogs.
Meanwhile, another 2013 study
presented some other interesting results. This study drew data from
multiple referral hospitals to determine the causes of death in spayed
or neutered versus intact dogs – and they found that spayed and neutered dogs, on average, lived longer
than intact dogs. Intact dogs were more likely to die of infectious
disease or trauma, while spayed or neutered dogs were more likely to die
of immune-mediated diseases or (again) cancer. In other words, while
spayed or neutered dogs did get cancer, it didn’t seem to shorten their
lifespans.
This study shed a new light on the cancer question. It suggested that
perhaps spayed or neutered animals might be more likely to get cancer
simply because they were living long enough to get it. Intact animals were more likely to die younger, perhaps simply not aging into the time of life when the risk of cancer rises.
So where does that leave us? Is there a causal link between
spaying/neutering and cancer? I think the question is still wide open.
What we really need is a study that follows animals forward throughout
their lifetimes instead of using retrospective records or surveys to get
the data – and, thanks to Morris Animal Foundation’s groundbreaking Golden Retriever Lifetime Study,
we are getting just that. This study is enrolling Goldens as puppies
and following their health over the course of their lives. It will be
years before the study gives us answers, but it provides hope for more
solid data. (Of course, it still can’t address the issue of bias, in
that owners who enroll their puppies in this study could be highly
responsible dog owners who provide excellent medical care!)
We can, however, do something about cancer in dogs without waiting
for the results of that study. It is no coincidence that two of the
studies discussed here investigated Golden Retrievers. Sixty percent of
Golden Retrievers will die of cancer. That is indisputably a problem
with the genetics of the breed, and other breeds suffer from similar
problems. We should be attacking cancer on all fronts, and this is a
front we don’t have to study first. Golden Retriever breeders are
between a rock and a hard place, trying to breed for health in a gene
pool which doesn’t have enough genetic diversity to support it. The
solution is to bring in new blood from gene pools with much lower risk
of cancer, breeding dogs who don’t look like purebred Goldens for a few
generations to revitalize the breed as a whole. Genetics contribute far
more to risk of cancer than whether an animal is spayed or neutered. We
clearly have a strong desire as a society to reduce the incidence of
cancer in Golden Retrievers and other breeds. While we’re studying risk
from spaying and neutering, let’s address the genetics question that we
know we can fix.
Image: Rob Kleine, Golden Retriever, Flickr Creative Commons License.
References
Torres de la Riva G, Hart BL, Farver TB, et al. Neutering Dogs: Effects
on Joint Disorders and Cancers in Golden Retrievers. PLoS ONE 2013. http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0055937
Zink MC, Farhoody P, Elser SE, et al. Evaluation of the risk and age
of onset of cancer and behavioral disorders in gonadectomized Vizslas.
Journal of the American Veterinary Medical Association 2014;244:309–319.
http://avmajournals.avma.org/doi/full/10.2460/javma.244.3.309 [Paywalled]
Hoffman JM, Creevy KE, Promislow DEL. Reproductive Capability Is
Associated with Lifespan and Cause of Death in Companion Dogs. PLoS ONE
2013. http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0061082
Friday, February 27, 2015
Monday, February 2, 2015
The rough guide to the fight-or-flight response
[Note: This post is intended as reading material for my upcoming online course, “Canine Hormones: From molecules to behavior.” This is an entirely online course offered through APDT, begins Februrary 11, and is worth 12 CEUs. I posted with more information. I encourage you to sign up!]
First, some terminology. I've been posting about the stress response recently. What's the difference between the fight-or-flight response and the stress response? It depends on who's talking. I like to use the term “stress response” to refer only to the hypothalamic-pituitary-adrenal (HPA) axis, best known for managing the levels of cortisol in the bloodstream. I use the term “fight-or-flight response” to refer to the sympathetic-adrenomedullary (SAM) axis, best known for managing the levels of adrenaline in the bloodstream. However, some people also refer to the SAM as the “stress response,” and some subdivide the two into the “slow arm of the stress response” (the HPA) and the “fast arm of the stress response” (the SAM).
The SAM is certainly fast! This is because it sends information straight from the brain to the adrenals through the nervous system instead of having to pass the message through a couple of other hormones first.
What it is: a subset of the involuntary nervous system, also known as the autonomic nervous system. The autonomic nervous system is subdivided into the sympathetic nervous system, which handles the fight-or-flight response, and the parasympathetic nervous system, which handles the rest-and-digest response.
What it does in the SAM: passes an electrical signal from the brain along the spinal cord and out to the adrenal glands.
The adrenals
What they are: small organs next to the kidneys responsible for sending all kinds of important hormones out into the body
What they do in the SAM: in response to input from nerves of the sympathetic nervous system, they release adrenaline (also known as epinephrine) and noradrenaline (also known as norepinephrine) into the bloodstream so that they can alert different organs and tissues around the body to the need to respond to a stressor fast, fast, fast. Note that the adrenals also release a hormone in the HPA axis. The adrenals are complicated little organs with different regions involved in the production and release of different hormones. In the case of the SAM, the interior region of the adrenals, the medulla, is the responsible party. The medulla contributes the M to SAM. (The outer layer of the adrenals, the adrenal cortex, is the active region in the HPA axis.)
Although this response is classically associated with fight (going on the offensive) or flight (getting away from a bad situation), another common behavior associated with this response is freezing: holding very still. This is a common response in some kinds of prey animals, like mice, but any species might react this way.
First, some terminology. I've been posting about the stress response recently. What's the difference between the fight-or-flight response and the stress response? It depends on who's talking. I like to use the term “stress response” to refer only to the hypothalamic-pituitary-adrenal (HPA) axis, best known for managing the levels of cortisol in the bloodstream. I use the term “fight-or-flight response” to refer to the sympathetic-adrenomedullary (SAM) axis, best known for managing the levels of adrenaline in the bloodstream. However, some people also refer to the SAM as the “stress response,” and some subdivide the two into the “slow arm of the stress response” (the HPA) and the “fast arm of the stress response” (the SAM).
The SAM is certainly fast! This is because it sends information straight from the brain to the adrenals through the nervous system instead of having to pass the message through a couple of other hormones first.
The sympathetic nervous system
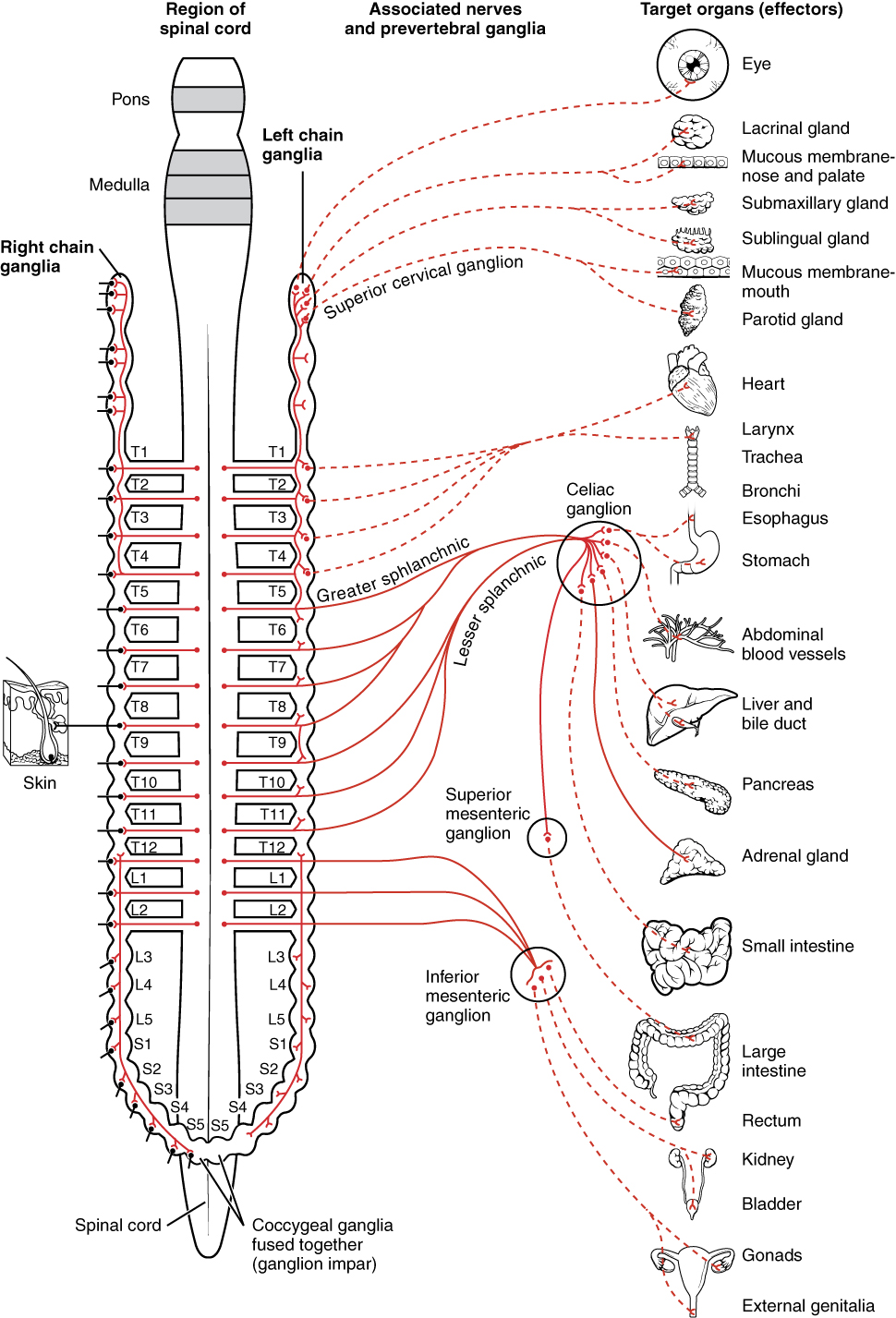 | |
| By OpenStax College [CC BY 3.0 (http://creativecommons.org/licenses/by/3.0)] via Wikimedia Commons |
What it is: a subset of the involuntary nervous system, also known as the autonomic nervous system. The autonomic nervous system is subdivided into the sympathetic nervous system, which handles the fight-or-flight response, and the parasympathetic nervous system, which handles the rest-and-digest response.
What it does in the SAM: passes an electrical signal from the brain along the spinal cord and out to the adrenal glands.
The adrenals
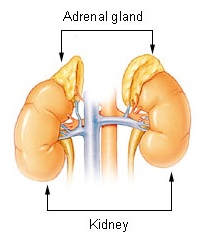 |
| By EEOC (cancer.gov) via Wikimedia Commons |
What they are: small organs next to the kidneys responsible for sending all kinds of important hormones out into the body
What they do in the SAM: in response to input from nerves of the sympathetic nervous system, they release adrenaline (also known as epinephrine) and noradrenaline (also known as norepinephrine) into the bloodstream so that they can alert different organs and tissues around the body to the need to respond to a stressor fast, fast, fast. Note that the adrenals also release a hormone in the HPA axis. The adrenals are complicated little organs with different regions involved in the production and release of different hormones. In the case of the SAM, the interior region of the adrenals, the medulla, is the responsible party. The medulla contributes the M to SAM. (The outer layer of the adrenals, the adrenal cortex, is the active region in the HPA axis.)
The minor players
The rest of the body
When adrenaline shoots into your bloodstream — well, you know what that feels like. Some people like the sensation; they are the types who seek out rollercoasters and horror movies. Some people hate it. Adrenaline tells your body to mobilize all its resources for a short term threat: your muscles get extra energy, the pupils of your eyes dilate to take in more light so you can see better, your heart beats faster and stronger, your lungs take in more air. It doesn't last long, just a minute or so.Although this response is classically associated with fight (going on the offensive) or flight (getting away from a bad situation), another common behavior associated with this response is freezing: holding very still. This is a common response in some kinds of prey animals, like mice, but any species might react this way.
The brain
What causes the fight-or-flight response to start? Different stimuli are scary to different individuals. I'm terrified of spiders and my cousin is terrified of snakes. On one particular walk in the woods she and I encountered one of each and took turns being scared and laughing at each other.The HPA axis
The HPA and SAM axes are intricately connected. If your SAM axis is triggered frequently, your HPA axis will start pumping out more cortisol — and if your HPA axis is chronically active, your SAM responses may become more intense. During the long chronic stress of veterinary school, one of my friends reported that she dropped a glass by mistake, and when it shattered, she screamed. The long-term high levels of cortisol in her bloodstream from the stress of veterinary school were affecting her adrenal medulla, making her adrenals pump out more adrenaline in response to acute stressors like the noise of breaking glass.
Subscribe to:
Posts (Atom)

